Paper
Within LASER, as part of the iMIT project, we focus on a special case of deep-seated vascular malformations as seen in identical-twin pregnancies that are complicated by the twin-to-twin transfusion syndrome (TTTS).
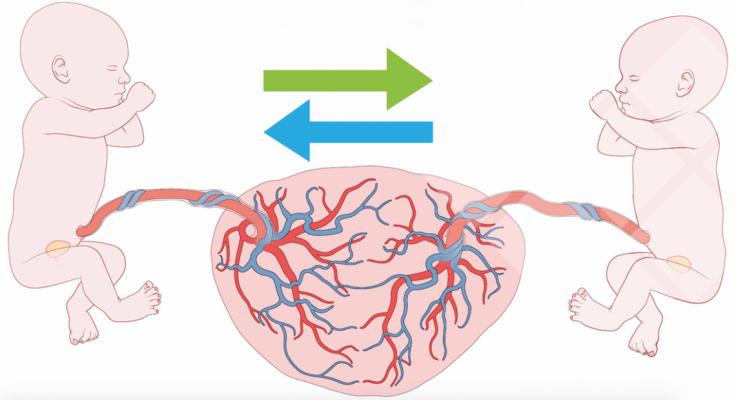
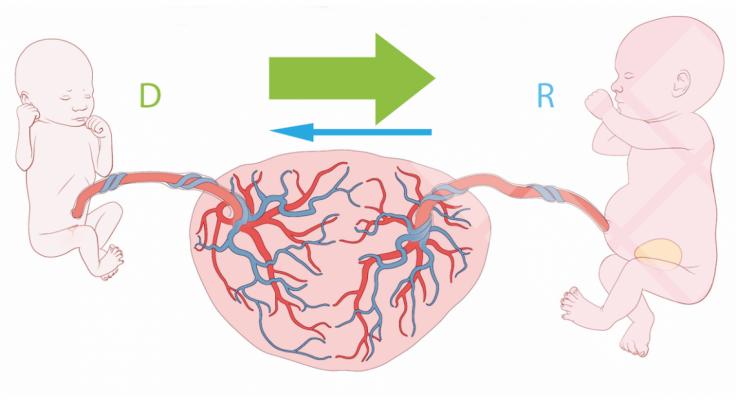
Due to erroneous interconnecting blood vessels (anastomoses) in the placenta, one twin receives too little blood while the other receives too much, so both are endangered.

Keywords
Twin-twin transfusion syndrome | Laser therapy | Laser power | Laser energy | Placenta
Authors & Partners
Joost Akkermans | Loes van der Donk | Suzanne H.P. Peeters | Sjoerd van Tuijl | Johanna M. Middeldorp | Enrico Lopriore | Dick Oepkes
Partners:
TU Delft - Dr. J.J. (John) van den Dobbelsteen
TU Delft - Dr. ir. Dennis van Gerwen
LUMC - Prof. Dr. D. (Dick) Oepkes
LUMC - J. (Joost) Akkermans MD, PhD
AMC - Prof. Dr. H.J.C.M. Sterenborg
Purpose of this study:
To assess the impact of laser power and firing angle on coagulation efficiency for closing placental anasto- moses in the treatment of twin-twin transfusion syndrome.
The treatment for TTTS is...
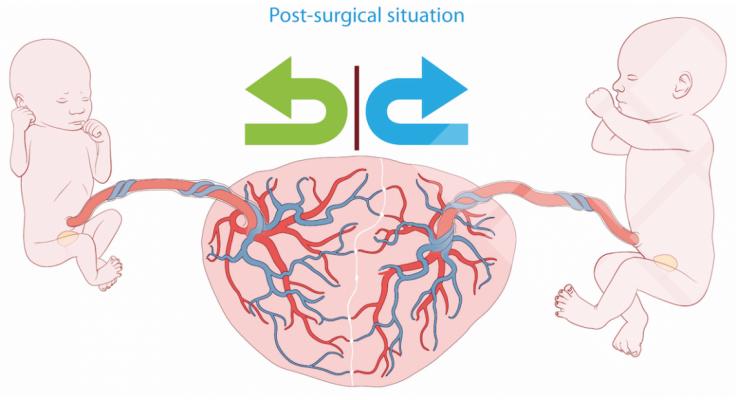
The treatment for TTTS is fetoscopic laser coagulation (FLC), which aims at closing off the vascular anastomoses. FLC involves puncture of the fetal membranes to gain access to the surface of the placenta from inside the amniotic sac. Important risk factors are the occurrence of residual anastomoses due to incomplete coagulation, and premature rupture of membranes.
To improve the outcome of these procedures physicians are in need of tools that can monitor the closure of the vessel during the procedure. Moreover, the development of instruments that allow laser coagulation in deep structures would enable approaching the anastomoses from the other side (i.e. through the placenta), thereby preventing puncture of the fetal membranes.
LASER Project
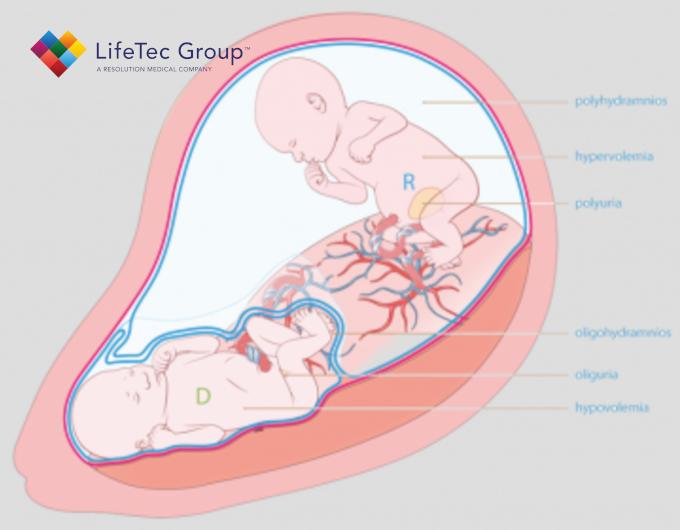
"Within LASER, as part of the iMIT project, we focus on a special case of deep-seated vascular malformations as seen in identical-twin pregnancies that are complicated by the twin-to-twin transfusion syndrome (TTTS).
Due to erroneous interconnecting blood vessels (anastomoses) in the placenta, one twin receives too little blood while the other receives too much, so both are endangered."
Abstract
Objective:
To assess the impact of laser power and firing angle on coagulation efficiency for closing placental anastomoses in the treatment of twin-twin transfusion syndrome.
Methods:
We used an ex vivo blood-perfused human placenta model to compare time to complete coagulation using 30 vs. 50 W of neodymium-doped yttrium aluminum garnet laser power and using a firing angle of 90° vs. 45°. Placentas were perfused with pig blood at 5 mL/min. Differences were analyzed using independent-samples t test, Mann- Whitney U test, or χ2 test as appropriate. Results: Coagulation took less time and energy using 50 W (n = 53) compared to30W (n=52), 11vs. 22s (p<0.001), and 557vs.659J (p= 0.007). Perpendicular coagulation (n = 53) took less time and energy compared to a 45° angle (n = 21), 11 vs. 17 s (p = 0.004), and 557 vs. 871 J (p = 0.004). Bleeding complicated 2 (3%) measurements in the 50-W group, 5 (10%) in the 30-W group, and 3 (14%) in the 45° group.
Discussion:
In a highly controlled model, a 50-W laser power setting was more energy efficient than 30 W in coagulating a placental vein.
In this research project...
In this research project a system was developed for treatment of deep-seated vascular malformations using laser coagulation while reducing damage to healthy tissue to a minimum.
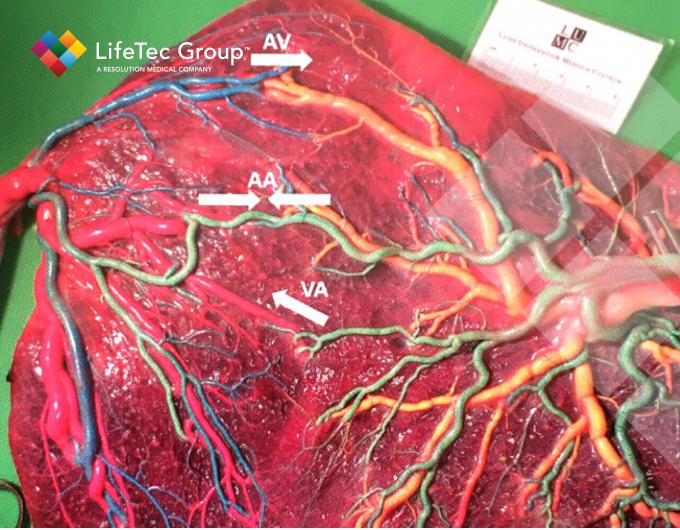
The main goal within LifeTec Group was to design and create a setup in which human placenta material could be subjected to laser treatment in order to characterize and optimize the laser coagulation process. In the developed set-up, placenta samples could be placed in a saline bath and kept at a steady 37°C temperature. The cannulated placenta veins were connected to the developed circulation system.
The laser fiber was kept in place by a system that allowed for easy and very accurate adjustment and was pointed at the vein either perpendicular or at a 45-degree angle. Fresh porcine blood was used to circulate in the placental vein. In this way accurate laser coagulations could be performed on the placenta material. This resulted in the first study reporting on laser coagulation efficiency of different power settings for obliterating superficial placental vessels.
To date, despite more than 25 years of laser surgery for TTTS, the ideal power setting for coagulation of anastomosis was unknown.
Download journal publication:
Testimonials
This research was supported by the Dutch Technology Foundation (STW), which is part of the Netherlands Organization for Scientific Research (NWO) and which is partly funded by the Ministry of Economic Affairs.
More about the iMit / Laser project: link
- COLOFON
Dutch Technology Foundation (STW)

Interested in more about what we do at LifeTec Group? Contact us!
Call at +31 40 2989393 Or e-mail us

